Chronic Low Back Pain And Its Complexities
Low back pain (LBP) or Lumbago is known to be one of the most widespread problems and conditions affecting a large population. It is considered a significant health problem, with the leading cause of discomfort and disability. Low back pain is long known to be complex, a multi-factorial disorder and one of the most common reasons for visits to primary care physicians and ER.
Low back pain has a significant economic burden in several western countries with a rise in healthcare costs. The pain condition can be compared to other conditions involving high costs, such as cardiovascular disease, cancer, and mental health disorders.
Chronic low back pain
Chronic low back pain(CLBP) is when low back pain persists for ≥12 weeks. CLBP can be very disabling to an individual and affects their functional, psychological, and social wellbeing, having a tremendous impact on society, from healthcare costs to personal life with a loss of productivity.
Low back pain causes and risk factors:
An underlying pathology or trauma can cause low back pain; however, in an estimated more than 85% of cases an underlying pathology or condition is absent, which then refers to as nonspecific LBP. Individuals with acute low back pain recover within a couple of days to weeks, while most of them experience persistent disabling symptoms leading to chronic pain symptoms.
In the absence of underlying pathology and biological reasons behind LBP, several risk factors can influence an individual’s chronicity of low back pain. Reasons vary and can include lifestyle factors like having sedentary life, sustained positions, and postures and heavy repetitive workload. Psychosocial factors such as an individual’s pain perceptions and expectations, depression, fear-avoidance beliefs, pain catastrophizing, low job satisfaction, cultural beliefs and previous experience of soreness all influence the chronicity of backaches.
A current evidence-based approach to low back pain:
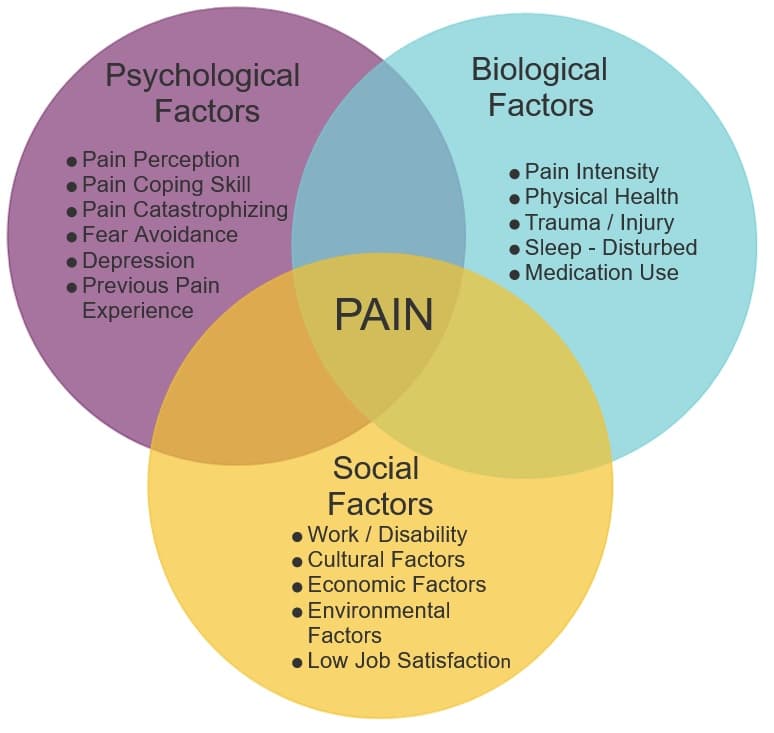
With several factors influencing chronic low back pain, a biomedical model of approach to management is usually a lost cause, which in turn led to the development of the biopsychosocial model of approach. Subsequently, the biopsychosocial method was developed to target several influencing factors that aim to improve the level of outcome and function in individuals suffering from chronic low back discomfort.
Current clinical guidelines recommend non-pharmacological interventions, including exercise therapy, general activity, cognitive behavioural therapy, and pain education for the management of persistent low back pain.
“If exercise could be packaged in a pill, it would be the single most widely prescribed and beneficial medicine in the nation.” -Robert Butler, National Institute on Aging.
Pain Neuroscience Education
However, believing staying active has not been helpful for recovery and for changing the outcomes. Still, a more psychosocial and behavioural approach may be required to improve individual treatment outcomes and reduce recurrence and to manage chronic low backache.
Pain neuroscience education is a cognitive-based intervention approach to inform individuals about what to expect from their ache, reduce the pathoanatomical model of focus, and focus on the factors that contribute to their soreness. There is a need to change the person’s belief system about aches and address factors such as recovery expectation, fear-avoidance, catastrophizing, and improve self-efficacy to influence Low back pain.
So, how do we use this approach in physiotherapy?
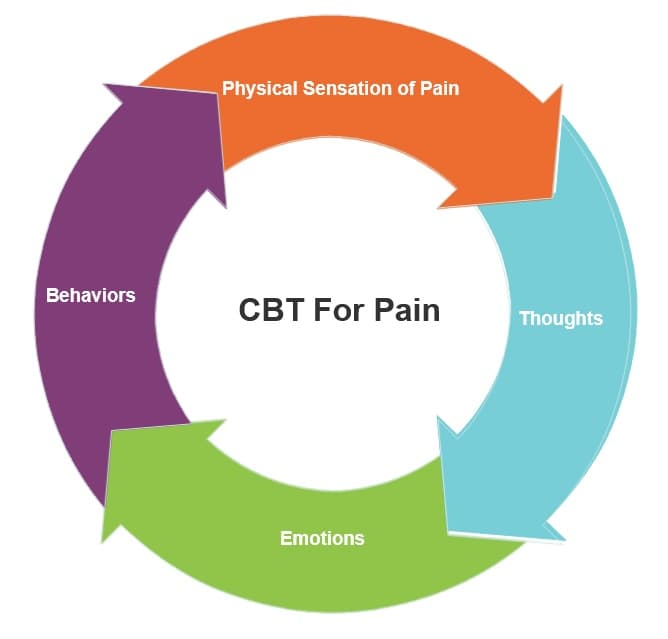
Within biopsychosocial treatment, cognitive-behavioural approaches are often used, such as graded exposure to activity, acceptance, and commitment therapy.
These interventions require a multidisciplinary approach for patients with moderate to high levels of disability.
Evidence suggests that every individual’s motivation and maintenance of self-management behaviours are essential and influenced by using an autonomous communication style to promote patient self-management in clinical practice.

Exercise therapy for low back pain
Various forms of exercise interventions are used to manage low back pain. Generally, any kind of exercise is beneficial, as exercise, in general, can improve soreness and function. Some studies have suggested that resistance training combined with flexibility training can be especially helpful compared to a passive treatment approach and coordination/ aerobic training. Resistance training is usually well tolerated by individuals with nonspecific low back soreness. It does not increase the risk of injury when it is approached and progressed in a graded manner. Another study reported that high-intensity exercise programs lead to a quick decrease in aches compared with low-intensity programs in the post-surgical population after lumbar surgery.
Remember, any form of exercise that improves and releases endorphins is excellent, as endorphins are a natural pain-relieving substance that our body can provide to us.

So, what can you do to help relieve the lower back pain?
Be Active! It is important to stay active despite your condition or aches. There is a hypothesis that physically being inactive may lead to a decrease in muscle strength and joint flexibility and, consequently, result in the joints being susceptible to further injuries. Physical activity is known to have numerous health benefits related to physiological and psychological well-being and health.
A study reported no association between low backache with high-level physical activity compared to low-level physical activity. Evidence has long shown that no one form of exercise is beneficial to general cardiovascular-based training, such as walking, jogging, running, swimming, and cycling, that has the same benefit of releasing endorphins, which can help reduce aches. Evidence has also shown that physiotherapy treatment for low back pain, yoga, meditation, and Pilates have the same benefits if you commit yourself to them.
Remember, movement is lotion for your joints and muscles. No movement, activity or exercise is superior to the other as long as you love the activity that you do and do the activity that you love and enjoy.
If you are struggling with low back pain and want to take back control of your life again, please see our highly trained physiotherapist who would be able to –provide you with an appropriate evidence-based treatment approach to your low backache problem.
References
Lisa Goudman, Eva Huysmans, Kelly Ickmans, Jo Nijs, Maarten Moens, Koen Putman, Ronald Buyl, Adriaan Louw, Tine Logghe, Iris Coppieters, A Modern Pain Neuroscience Approach in Patients Undergoing Surgery for Lumbar Radiculopathy: A Clinical Perspective, Physical Therapy, Volume 99, Issue 7, July 2019, Pages 933–945.
Matthews J, Hall AM, Hernon M, et al. A brief report on the development of a theoretically grounded intervention to promote patient autonomy and self-management of physiotherapy patients: face validity and feasibility of implementation. BMC health services research. 2015; 15:260. doi:10.1186/s12913-015-0921-1.
Alshehri MA, Alzahrani H, Alotaibi M, et al Physiotherapists’ pain attitudes and beliefs towards chronic low back pain and their association with treatment selection: a cross-sectional study BMJ Open 2020;10: e037159. doi: 10.1136/bmjopen-2020-037159
Tjøsvoll, Svein O et al. “Periodized resistance training for persistent nonspecific low back pain: a mixed methods feasibility study.” BMC sports science, medicine & rehabilitation vol. 12 30. 8 May. 2020, doi:10.1186/s13102-020-00181-0
Koppenaal T, Arensman RM, van Dongen JM, et al. Effectiveness and cost-effectiveness of stratified blended physiotherapy in patients with nonspecific low back pain: study protocol of a cluster randomized controlled trial. BMC musculoskeletal disorders. 2020;21(1):265. doi:10.1186/s12891-020-3174-z.
Matsudaira, Ko et al. “Assessment of risk factors for nonspecific chronic disabling low back pain in Japanese workers-findings from the CUPID (Cultural and Psychosocial Influences on Disability) study.” Industrial health vol. 57,4 (2019): 503-510. doi:10.2486/indhealth.2018-0157
Alzahrani, Hosam et al. “The association between physical activity and low back pain: a systematic review and meta-analysis of observational studies.” Scientific reports vol. 9,1 8244. 3 Jun. 2019, doi:10.1038/s41598-019-44664-8

Cynthia Pathipati – Registered Physiotherapist
Cynthia Pathipati completed her bachelor’s in physiotherapy and is a qualified Registered Physiotherapist in good standing with the College of Physiotherapists of BC with more than 15 yrs of experience. She has Post-Graduate Credentials and Certifications as well as extensive knowledge experience in treating pelvic floor, orthopedic, neurological, vestibular and pain conditions.