Understanding Frozen Shoulder – A Complete Guide
Understanding frozen shoulder – What is it?
Adhesive Capsulitis or more commonly known as Frozen Shoulder (FS), is considered a musculoskeletal condition, with 3-5% being affected in the general population. It has a significant impact on the daily activities of the patient’s life.
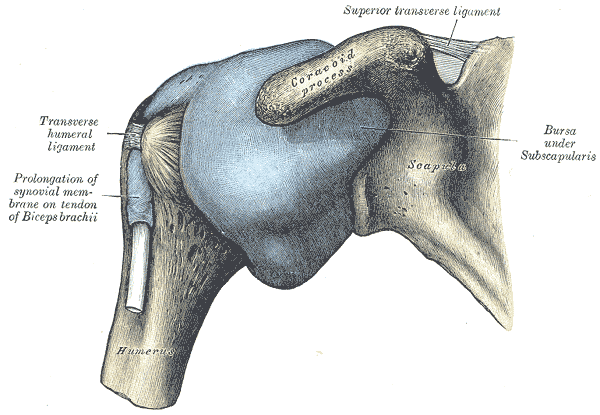
Duplay in 1879, first described the frozen shoulder as “humeroscapular periarthritis”. In 1934 the term “frozen shoulder” was introduced by Codman and is still widely in use. He described the condition as “difficult to define, difficult to treat and difficult to explain,” and this remains true to this day (Ryan, Victoria et al. 2016). In 1945 Adhesive capsulitis was termed by Neviaser when he described the texture of the joint capsule as “adhesive” due to inflammatory and fibrotic changes observed in the capsule or bursa.
Classification of frozen shoulder
Primary/ Idiopathic FS: usually associated with other diseases and conditions like diabetes and thyroid diseases or Parkinson’s disease etc. It is often an insidious onset.
Secondary FS: can occur following a trauma (fracture, dislocation, or soft tissue injury) and immobilization following rotator cuff tendon tear, Impingement, biceps tenosynovitis and calcific tendonitis.
Studies have shown that the increased pain from the shoulder pathology is said to cause reduced movement in the shoulder leading to a frozen shoulder. The pain can increase the reluctance to move to cause neurological inhibition and leading to a frozen state. It can explain why FS is common after a shoulder injury.

Risk factors associated with frozen shoulder
Diabetes Mellitus – Frozen shoulder is known to commonly occur in patients with specific comorbidities, of which is more common being diabetes. Several studies reported an increased incidence in patients with diabetes, from 10-40% (Su, Yu-De et al.,2019). The study also noted that diabetic FS patient’s symptoms were found to be more persistent and were difficult to treat with a decreased functional outcome than nondiabetic FS (Le, HV et al., 2017)
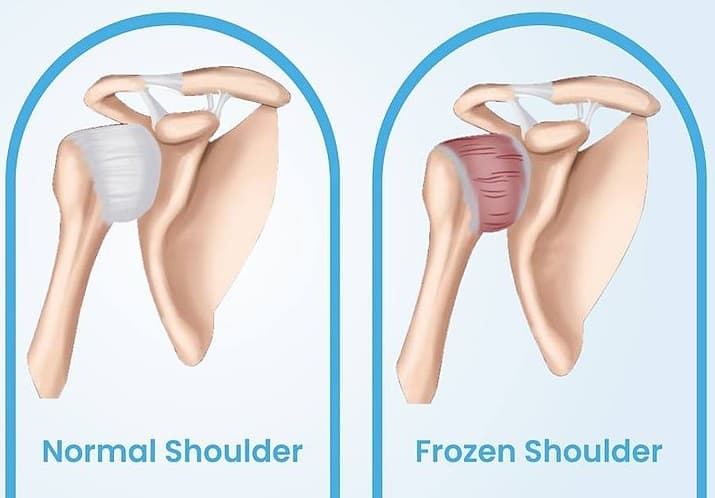
Frozen shoulder symptoms:
Evaluation of frozen shoulder:
The X-Ray results showed no significant findings in the history of the patient’s condition or radiographic evaluation where osteopenia or calcific tendonitis were absent. (Abrassart S. et al. 2020) To explain the movement loss or pain.
The absence of definitive diagnostic criteria brings a challenge for diagnosing and managing. Other problems like rotator cuff tendinopathy, calcific tendonitis, and early glenohumeral arthritis can also resemble closely frozen shoulders in the early stages and challenge the diagnosis.
A recent study suggested that the thickening of the joint capsule, coracohumeral ligament and synovium is a feature of a frozen shoulder. However, there is not enough data from imaging studies to specify the articular changes associated with this condition. (Ryan, Victoria et al. 2016).
MRI with IV contrast injection can be helpful for the diagnosis of FS under challenging cases. The intensity of enhanced signals in the rotator cuff interval seems to be related to the early stage of the frozen shoulder (Pessis E et al. 2020).
Phases of frozen shoulder:
Frozen shoulder is usually reported as a self-limiting condition and is described in three phases:
This long recovery period affects patients’ routine life, occupational performance, and recreational activities.
A recent study noted that the description of the disease in a ‘three-phase or self-limiting condition is to be avoided. It helps to reduce distress and potential harm as most of the population affected by FS does not follow the described phase of resolution nor the time frame, even with appropriate treatment. The recommendation is based on available evidence and the natural history of the condition as “which often sees short-term improvement, but which bears a high chance of ongoing low-level restriction and pain.” (Abrassart S. et al. 2020)
A related area of interest to read: Ankle Sprain Problem, Management and Recovery.

Management for frozen shoulder:
Most frozen shoulder patients experience resolution with a conservative management approach, and thus it has been the first line of management. Initial conservative management is known to be successful in up to 90% of patients. Appropriate treatment is usually required for a return to their life and function. However, definitive treatment strategies have not been established, and several management strategies are in use.
Conservative management can include:
Surgical interventions for frozen shoulder:
Patients who are regressing or not making improvements despite appropriate therapy are likely to require surgical intervention. Surgical intervention for FS at 2.67 procedures per 10,000 general population in a year. Surgical management of FS varies substantially and is highly based on personal experience and training rather than evidence (Cho CH et al. 2019)
Physiotherapy treatment for frozen shoulder:
Physiotherapy is widely accepted in the conservative management of Frozen Shoulders. Several studies have demonstrated physiotherapy as an adjunctive intervention in providing excellent results.
NSAIDs were more effective when used combined with physiotherapy compared to NSAIDs alone. Steroid injection, in conjunction with physiotherapy, provided better outcomes compared to intraarticular injection alone.
Home exercises for frozen shoulder and physiotherapy are a common first-line treatment for frozen shoulder.

In the freezing phase (2-9 months), pain is quite predominant, and steroid injection provides rapid pain relief in the short-term period with an Active assisted range of movement as tolerated.
During the frozen phase (4–12 months), physiotherapy focused on increasing ROM, such as mobilization techniques (limited evidence).
In the thawing phase (12–42 months), progressive improvement in ROM, strength and functional retraining or rehabilitation. As pain with muscular inhibition usually results in compensatory movements, the adaptation of scapular motion is essential in managing rehabilitation in FS.
Mobilization, Progressive Therapeutic exercises, and functional neuromuscular training are strongly recommended for improving pain, range of motion and function during the 2nd and 3rd phases of the frozen shoulder.
Therapeutic modalities for frozen shoulder:
- Studies have noted that Low-level laser therapy was effective for pain relief but moderately suggested for improving function and was not recommended for improving ROM.
- Acupuncture with therapeutic exercises – is moderately recommended for pain relief, ROM, and function.
- Continuous passive motion was recommended for short-term pain relief but did not improve ROM or function.
- Deep heat may be used for pain relief and to improve ROM.
- Therapeutic Ultrasound for pain relief and improving ROM or function is not recommended and delays the improvement (Jain TK et al. 2014). The study also noted that adding an ultrasound treatment modality did not provide any additional benefits for the treatment of the frozen shoulder.
- Extracorporeal shockwave therapy (ESWT) – few studies have found some decrease in pain and slight functionality improvements (forward ROM) through the administration of ESWT with Fascial manipulation (Yuan X et al. 2018). However, to determine whether the recovery is enhanced by a supervised exercise program or on its own or combined with ESWT-FM, additional research and prospective randomized, blinded, controlled clinical trials must be conducted and are still lacking at this time.
- High-intensity Laser Therapy (HILT): Study noted that HILT (a non-invasive procedure) provided significant pain relief at 3 and 8 weeks but not at later stages. Further study is still required.
Studies and literature reviews have shown that most patients with frozen shoulder experience resolution of symptoms with conservative management. It is, however, essential to be able to tell a patient with some confidence that an idiopathic frozen shoulder generally recovers well without any restriction in range of motion or pain (Vastamiki Heidi et al. 2012)
If you think you have a frozen shoulder or are developing one, see your physician or your physiotherapist for a physical exam and exercise program to manage and help the condition. Call Opal Physiotherapy in Langley, B.C, if you need further information or to book an appointment.
Need to treat your frozen shoulder? Learn more about our physiotherapy for frozen shoulder treatment, or book an appointment with our Physiotherapist at 604-532-7887

Cynthia Pathipati – Registered Physiotherapist
Cynthia Pathipati completed her bachelor’s in physiotherapy and is a qualified Registered Physiotherapist in good standing with the College of Physiotherapists of BC with more than 15 yrs of experience. She has Post-Graduate Credentials and Certifications as well as extensive knowledge experience in treating pelvic floor, orthopedic, neurological, vestibular and pain conditions.