Patellofemoral Pain Syndrome – Pain In The Knee
Patellofemoral pain syndrome
Knee pain is one of the common conditions that are prevalent in the general population. Patellofemoral pain syndrome (PFPS) is one of the commonly diagnosed knee conditions, it is also known by its name as Anterior knee pain or Runner’s knee. It affects approximately 23% of adults, 29% of adolescents and is more frequent in women (Yanez-Álvarez et al. 2020) and athletes. Patellofemoral pain (PFP) is prevalent in adults under the age of 40. The long-term prognosis is poor for PFPS. Approximately one-third of patients are pain-free in one year, and 91% still report soreness and dysfunction four years after onset. (Benjamin E. Smith et al., 2019)
Soreness in and around the knee and behind the kneecap with weak muscles usually causes reduced function in the knee, impacting daily activities, quality of life and sports.
Diagnosis is usually done based on the clinical history and requires ruling out any injury to ligaments or menisci in the knee. Patellofemoral syndrome is often a multifactorial problem.
Patellofemoral pain syndrome is a diffused soreness in front of the knee or below the kneecap, usually unrelated to any trauma or no known specific cause.
Physical therapy can help Patellofemoral syndrome by improving the strength and flexibility of the muscles around the knee. This can help to decrease the amount of stress on the patella (kneecap) and improve the alignment of the knee joint. A physical therapist can also help to improve your range of motion and reduce pain.

Common symptoms of patellofemoral pain syndrome:
The most common symptom associated with Patellofemoral Pain Syndrome is soreness in or around the anterior patella that increases when the knee flexion occurs during loading activities.
- Swelling in the knee
- Knee clicking or grinding
- Soreness increases with activities like prolonged sitting, walking downhill, walking downstairs, squatting, kneeling, hiking etc.
- Pain is usually relieved by stopping the activities
Potential causes of patellofemoral disorder:
Muscle insufficiency: Muscles are unable to provide or exert a normal force for a typical movement pattern to occur. There is an associated cramping sensation as the muscles are unable to shorten or lengthen to allow full joint movement. Muscle insufficiency usually is caused by a combination of weak or tight muscles.
Overuse Syndrome: Performing repeated activities and sports that require repeated bending of the knees like repeated squatting, and jumping, causes an increased risk for PFPS.

Muscle Overload: A sudden increase in activity level without proper training (running) can cause an increased load to the patella that is more than usual, leading to anterior knee soreness.
Foot Wear: Wearing inappropriate footwear during training/ exercises can also lead to knee problems.
Trauma: Direct trauma to the kneecap during sports-related activities or falls can lead to PFP.
Associated factors for patellofemoral pain syndrome:
Many patients with Patellofemoral Pain syndrome develop associated pain such as fear-avoidance, catastrophizing thoughts, and low self-efficacy. These factors affect the function and quality of life of patients and alter their individual pain experience, which often leads to a chronic pain state. A systematic review found self-efficacy and depression were among the most substantial prognostic factors for pain and disability regardless of the intervention used (Benjamin E. Smith et al. 2019). Based on this foundation, the interventions aim to improve pain-related fear and movement through education and gradually increase physical activity with self-management strategies.
Management of patellofemoral pain syndrome:
- Avoid prolonged resting or inactivity. Perform activities as tolerated during the day, like short walks, cycling, swimming etc.
- Temporarily avoid deep squats and kneeling.
- Temporarily restrict running and prolonged walking and reduce the intensity of activity as tolerated.
- Avoid prolonged sitting with the knee in the bent position; instead, try moving the knee several times, bending and straightening the knee 5-10 times every 15 minutes while you are sitting.
- Wear appropriate footwear. Avoid wearing high heels, sandals and shoes that lack adequate foot support.
- Avoid strenuous knee extension exercises during gym training.
- Regularly perform warm-ups and stretch before and after any activity or exercise.
Treatment for patellofemoral pain syndrome:
With the knowledge that PFPS is multifactorial, it is all-important to recognize that every patient with PFPS is distinctive and will require an individualized treatment approach.
Multi-modal nonoperative therapy with short-term use of NSAIDs, taping and bracing to the patella. Exercise therapy, including knee strengthening, core training, and hip and trunk muscle training, has shown to be the best course of treatment to manage PFPS.
Injections remain a commonly used treatment for knee soreness; however, the evidence for their use in PFPS is still limited.
Surgical Interventions are typically not performed due to a wide range of effective conservative treatments available for PFPS. Most surgical interventions are aimed at treating malalignment or injured cartilage. Surgical consultation for PFPS is usually considered for those patients whose symptoms persist past 6-12 months of conservative management of home exercises and active rehabilitation and in the case of severe instability in the knee.
To explore a related area of interest, read: pelvic floor muscle training for athletes.
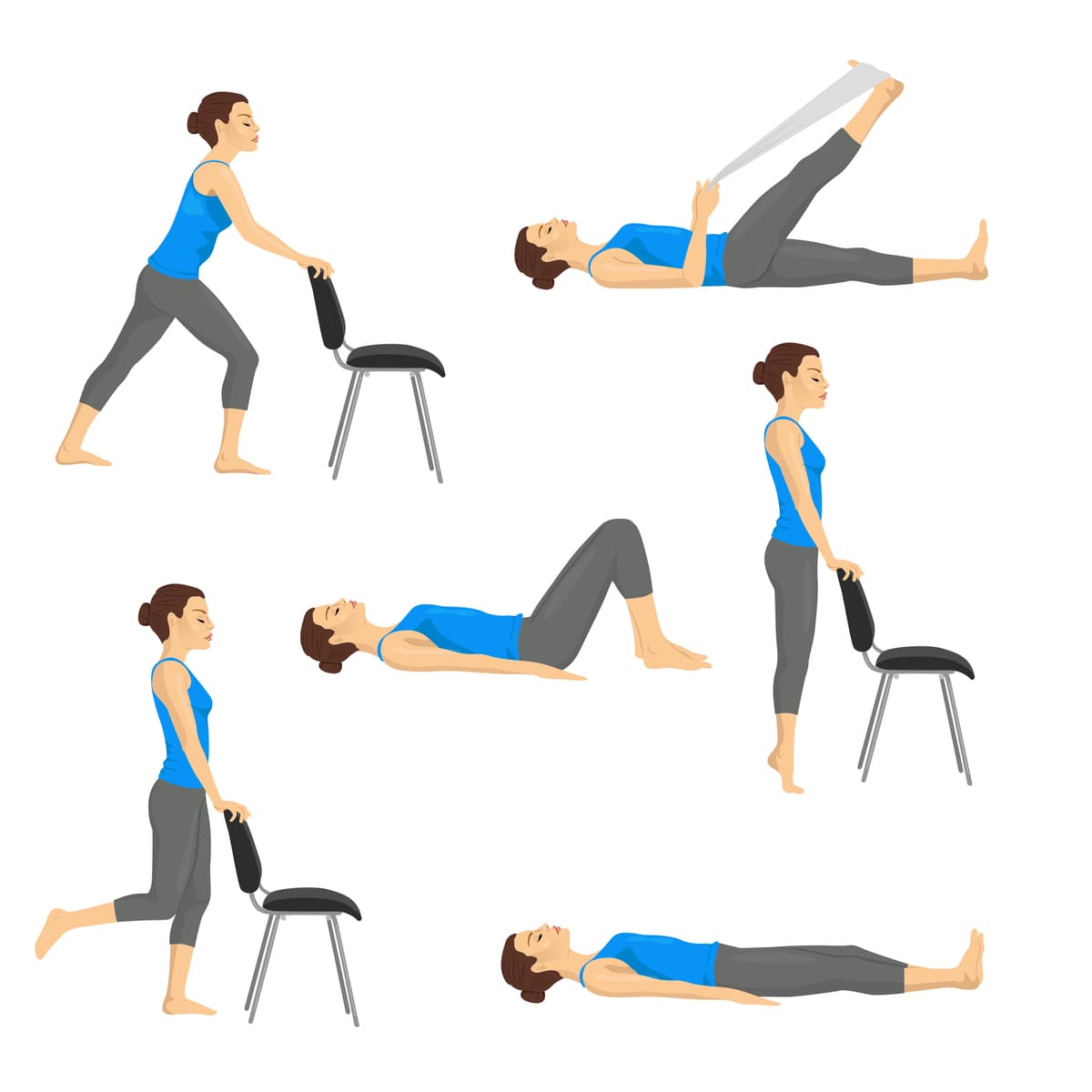
Patellofemoral pain exercises
Exercise therapy is an evidence-based conservative approach often prescribed for PFP. There is strong evidence that supports strength training as part of exercise programmes for conventional treatment, to obtain better results in terms of soreness reduction and improved function.
A loaded self-managed exercise programme designed around pain education and self-management strategies is feasible and is all acceptable for PFP (Benjamin E. Smith et al., 2019)
How can a physiotherapist help treat patellofemoral pain?
A Physical therapist can help with patellofemoral pain syndrome by assessing the individual and developing a treatment plan. A physiotherapist also helps patellofemoral pain syndrome by helping to stretch and strengthen the muscles around the knee, exercises and massage. They can also help improve the knee’s alignment and teach you how to properly use your muscles when moving your knee. They can also provide education on how to prevent further pain and injury.
Physical therapists will perform an assessment and provide treatment for patellofemoral pain based on the findings and will often include pain education, manual therapy, mobilization, and taping of your knee. Also providing physiotherapy-based exercises to retrain your muscles and improve flexibility and muscle strength in your lower extremity. As the pain reduces, the workouts are usually progressed and challenged based on your activity level and needs. You may also be recommended for a brace or to see an orthotist for consultation if required.
Please consult our physiotherapist if you are experiencing Patellofemoral Pain Syndrome.

Cynthia Pathipati – Registered Physiotherapist
Cynthia Pathipati completed her bachelor’s in physiotherapy and is a qualified Registered Physiotherapist in good standing with the College of Physiotherapists of BC with more than 15 yrs of experience. She has Post-Graduate Credentials and Certifications as well as extensive knowledge experience in treating pelvic floor, orthopedic, neurological, vestibular and pain conditions.